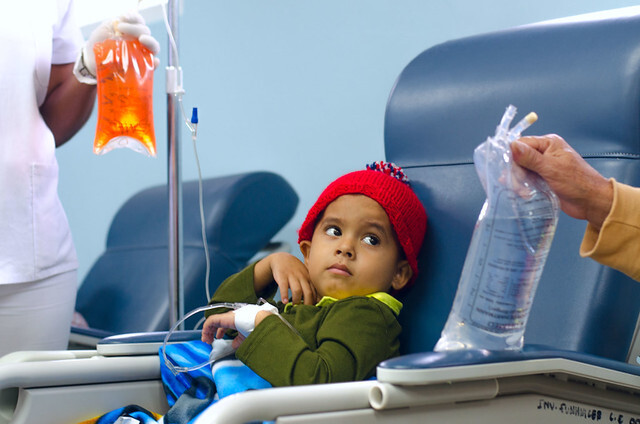
Chemotherapy treatment uses anti-cancer medicines (drugs) to treat cancer by stopping cells from growing, or by destroying cells.
Key points to remember
- chemotherapy treatment uses anti-cancer medicines (drugs) to treat cancer by stopping cells from growing, or by destroying cells
- your child may have several types of chemotherapy
- each type of chemotherapy medicine stops cell growth or destroys cells in a different way
- how your child receives chemotherapy will depend on the type of cancer they have and the chemotherapy medicines that work best for that type of cancer
What is chemotherapy?
Chemotherapy treatment uses anti-cancer medicines (drugs) to treat cancer by stopping cells from growing, or by destroying cells.
Your child may have several types of chemotherapy because each type of chemotherapy medicine stops cell growth or destroys cells in a different way.When chemotherapy destroys cancer cells, it can also damage healthy cells. This damage can cause side effects. Often, the side effects get better or go away once the chemotherapy treatment ends. Different drugs have different side effects. Each child can react differently to the same chemotherapy drug.
Your child may receive chemotherapy treatment:
- by mouth
- into a vein
- into a muscle
- into the spinal fluid
What medicines will my child have during chemotherapy?
Soon after your child's cancer diagnosis, your child's healthcare team will give you a treatment plan, often called a treatment protocol.
This will have details of the treatment and the names of the medicines the doctors will use. It will also explain how and when the medical team will give the medicines.
Your child's healthcare team will also give you information sheets about the medicines that your child will have and the possible side effects. The information sheet will also tell you if you need to protect you and your family from contact with these medicines. This is because some medicines stay in wee (urine), poo (faeces) and blood up to 48 hours after chemotherapy treatment ends.
In most cases, chemotherapy happens in cycles. A cycle is a period of chemotherapy treatment followed by a rest period. The rest period allows time for your child's body to build healthy new cells before the next treatment. For example, your child may have chemotherapy for 1 week and then have 2 weeks of rest. These 3 weeks make up 1 cycle.
Your child's healthcare team will give you information about your child's chemotherapy schedule. They will also list all the chemotherapy medicines that your child will have.
What about safety with chemotherapy?
After your child has chemotherapy, their body sometimes gets rid of small amounts of the drugs in body fluids including blood, wee, poo or vomit. The amount will vary depending on the kind of drug they have.
- get rid of wee, poo and vomit in the toilet - flush twice with the lid down to avoid splashing
- put soiled disposable nappies in a plastic bag and put them in the rubbish
- do a separate wash of other dirty things like cloth nappies, linen and clothing – use lots of detergent and water
- make sure you wash hands thoroughly after handling wee, poo and vomit
- wear gloves when handling wee, poo and vomit if you are pregnant and/or breastfeeding
What are the side effects?
Many chemotherapy medicines cannot tell the difference between normal cells and cancer cells. These medicines affect all cells that divide rapidly. The damage to normal cells may lead to side effects. Different chemotherapy medicines cause different side effects.
Since children respond to chemotherapy differently, some children will experience more side effects than others. Your child's healthcare team will manage the side effects, as they develop, to keep your child as comfortable as possible. Because normal cells can repair themselves, the side effects are nearly always temporary.Chemotherapy medicines most often affect the normal cells in the:
- bone marrow (where blood is produced), causing fewer blood cells than normal - this is known as a low blood count
- digestive system (mouth, stomach, bowels or intestines, rectum) causing nausea, vomiting or mouth and gut ulcers
- hair follicles, causing hair loss
What can I do?
Tell your child's doctor or nurse if you think the medicine is causing other side effects.
Keep all your medicine information sheets for your child and file them together in a folder. They list the possible side effects of your child's medicines.
Keep the treatment plan (treatment protocol) for your child and file this together with your child's medicine information sheets and any other printouts about your child's treatments.
Will chemotherapy hurt?
Oral chemotherapy
Oral chemotherapy is just like taking any other medicine by mouth. It does not hurt but if your child does not like medicines, the nurse or hospital play specialist will give you some hints to help make it easier for them.
You may be able to give chemotherapy to your child by mouth at home. If this is an option, the nursing staff or pharmacist will teach you about this.
Injections into muscle
A doctor or nurse may inject the medicine into your child's muscle (intramuscular injection). This may sting.
Injections under the skin
A doctor or nurse may give an injection under your child's skin (subcutaneous injection). If this happens, your child's nurse will first put a numbing (anaesthetic) cream on your child's skin. This will make the area feel numb. Either a nurse will put the cream on your child's skin, or show you how to do it yourself.
Injections into the spinal cord fluid
If your child needs an injection into the fluid around the spinal cord (intrathecal injection), this will happen under general anaesthetic so your child will be asleep and will not feel anything.
Injections into a vein
If your child has an external catheter, a nurse will put the medicine into the tubing so there is no skin prick.
If your child has an internal catheter, you or a nurse can put an anaesthetic cream on your child's skin over the port. This will numb your child's skin before the nurse puts the needle in.
Will my child need to have treatment in hospital?
Not always.
Your child can have chemotherapy tablets or liquid (suspension) at home.Your child may receive some kinds of chemotherapy at an outpatient clinic or day-stay unit of the hospital. Your child may receive the medication:
- as a quick injection from a syringe or
- in a bag of fluid over several hours
Click Donate to fund the ongoing development of the Circulating Tumor DNA project which will improve outcomes for those children already diagnosed with cancer.
Disclaimer - Content on this blog is for educational use only. Please consult your doctor or other health professional to make sure the information is right for your child.
Copyright - Please note that the information on this blog is copyright owned by The Paediatric Society of New Zealand and Starship Foundation. See copyright information at the Kids Health website.